Hospitals Compare Abstracted and Electronic Measures: Which is a better reflection of care?
By Erin Heilman September 1, 2017 Regulatory Updates: Hospital

For years, hospitals have relied on manually abstracting their quality measures to get an accurate picture of their hospital’s quality of patient care. Over the last five years or so, the attention has shifted to Electronic Clinical Quality Measures or eCQMs. This shift has intensified since 2016 when CMS, followed by The Joint Commission, started requiring eCQM data submission to successfully complete their quality reporting programs.
This left us wondering, “how do hospitals feel about their chart-abstracted measures in light of this inclusion of eCQM data?”
This week, we reveal the results of our recent survey of Medisolv hospitals and how they feel about these two types of quality measures.
How do hospitals feel about their chart-abstracted measures?
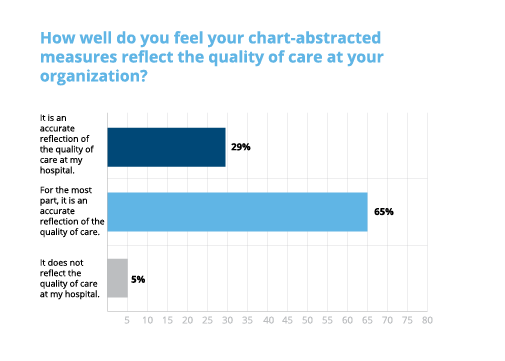
One of the most striking observations from the survey results is that the overwhelming majority of respondents felt confident in their chart-abstracted measure results. 95% of people surveyed feel that, for the most part, their chart-abstracted measure results accurately reflect the quality of care at their organization.
What’s more, is that the majority of hospitals feel that their measure results are better than they were five years ago. I should mention that the majority of respondents have been working in this field for over 10 years.
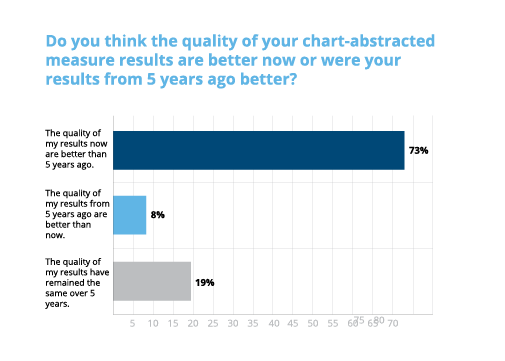
How have chart-abstracted measures changed over the last five years?
What are some reasons for the better results? Well a couple of industry changes could be responsible for the change. Respondents pointed toward a few common themes: better technology, less measures to abstract and better physician compliance.
Respondent: "Less measures are chart abstracted."
Let’s take a step back. Do you all remember 2012? Do you remember what it was like to abstract during that time? When the 2012 IPPS final rule dropped, CMS required that 43 measures be abstracted and reported as a part of the Inpatient Quality Reporting (IQR) program. Do you know how many chart-abstracted measures are required today? Six.
Also see: Download the Ultimate Regulatory Reporting Kit (CMS and The Joint Commission quality program requirements.)
The fact that there are less measures to abstract certainly seems to be a factor. Additionally, the progression of new and better technologies has helped.
Respondent: “Due to new technology for abstraction tools, which makes core measure abstraction more efficient."
Hospitals are more confident in their chart-abstracted measure results.
When asked if they felt their chart-abstracted measures results were better than their eCQM counterparts, the answers were less clear. Nearly half of the participants surveyed weren’t sure which measure results were better. However, there was a significant chunk (42%) of respondents who felt that their chart-abstracted measures are still better than their eCQM results.
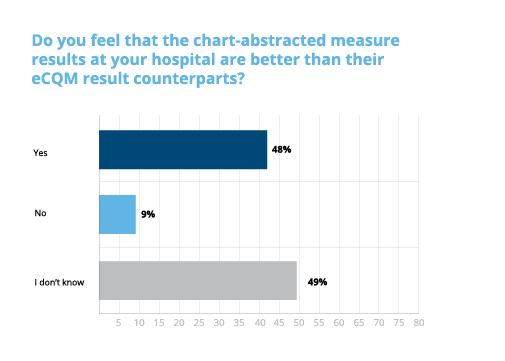
What’s clear is that … we’re not clear. Hospitals are in a state of change. eCQMs have been advancing over the last few years, but leadership remains hesitant to fully rely on eCQM results.
Five years from now will people say that their chart-abstracted measures are still a more accurate reflection of the quality of care at their hospital? Or will eCQMs have improved enough over that span of time to win the confidence of the Quality director or other leadership?
Some think their job got easier over the last five years, while others felt it got harder.
Another interesting result from this survey was the perception of how their job has changed over the last five years. Keep in mind that 57% of the people who responded had a job title that was specifically focused on abstraction. While 37% were at the Director level and most of those specifically for the Quality department.
Some people felt that their job became easier over the last five years and some felt it became harder.
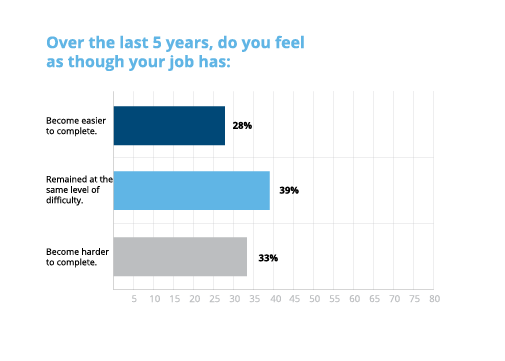
It seems that whether they picked harder or easier depended upon which aspect of their job they were thinking about.
The job got easier
For instance, of the 28% of people who believed their job became easier, their comments were similar to those who felt their core measure performance results improved over the last five years.
Because there were less core measures to abstract, coupled with advancements in technologies, their job became easier to complete. In fact, of those who commented as to why their job became easier, 87.5% pointed to advances in technology that have helped them to complete their charts easier.
Respondent: "Electronic abstraction worksheets have made it far less cumbersome than abstracting manually."
The job got harder
Of the 33% who said their job has become harder to complete, 47% said it was because of the changes and increases in regulations for all CMS programs. And if you factor in those people who said their job responsibilities have increased, the number raised to 67%.
Respondent: "There are many more requirements to keep up with to meet current regulations."
Respondent: "We are constantly asked to be the subject matter experts for various patient populations ... There is always more work with fewer resources available to care for patients."
It seems that those who were traditionally in charge of abstracting measures are taking on more responsibilities with less resources to manage their workload. In fact, 61% of those surveyed were also responsible for monitoring and improving the performance of their hospital’s eCQM results.
A few observations from common-themed comments.
After reviewing the comments, there were a couple of themes that emerged over and over again.
What they hate the most
I would be remiss if I didn’t mention the nasty 6-letter curse word: Sepsis. This comment popped up everywhere we asked for additional comments.
Respondent: “The Sepsis core measure is so complex … my productivity has been significantly reduced. It’s been difficult to implement the Sepsis criteria into patient care, which has left us with multiple places to search for information in the patient record.”
Respondent: “The Sepsis measure is complex and time consuming.”
Respondent: “My job has become harder to complete because of the Sepsis measures.”
Respondent: “The Sepsis measure set is ridiculously complex in abstracting rules with unrealistic expectations for physician documentation.”
Respondent: “SEPSIS!”
It seems that while the number of measures required to abstract has decreased, the addition of the Sepsis measure set has significantly burdened abstractors. Maybe I should start an “I Hate the Sepsis Measure” Facebook group. We could all do a little virtual group therapy.
Bridging the gap between eCQMs and patient care
A few hospitals felt that eCQMs created a process culture where physicians were simply checking the box instead of thinking about the quality of care.
Respondent: “The nurses and doctors are having to balance bedside care with checking the correct box to get reimbursed for their hard work.”
So, while the actual eCQM results do seem to be gaining the confidence of those responsible for hospital performance, some hospitals still feel concern about the value of eCQMs. Ultimately, electronic quality measures should drive performance improvement and make patient care better in your hospital. But until your eCQMs start holding their own, hospitals will still continue to question their value.
Join us for an upcoming webinar about using your eCQMs to improve performance and see how you can go from eCQM uncertainty to eCQM excellence.
[DOWNLOAD]
IQR Measure Removal Guide: 2019-2021
Hospitals, providers and healthcare organizations have been vocal over the years about the burden they feel related to all of these regulatory programs and data capture requirements.
In an effort to reduce the reporting burden, CMS plans to eliminate 39 measures between 2019 and 2021.
This measure removal guide provides a full list of all the measures in the IQR program and their plan for retirement or retention.






Add a comment