What are dQMs?

A new healthcare abbreviation is entering the quality improvement nomenclature: dQMs. What are they and how soon will they be here? Dr. Zahid Butt, Medisolv's CEO, explains.
If you've worked in healthcare for any length of time, you know that the list of abbreviations and acronyms we all regularly use, especially in the quality improvement world, is quite long. In many ways, we speak our own language. Now, a new entry is added to the quality improvement dictionary: digital quality measures, or dQMs.
Let me explain what dQMs are and how they might affect your work in quality management at your hospital, health system or medical practice.
dQM vs. eCQM
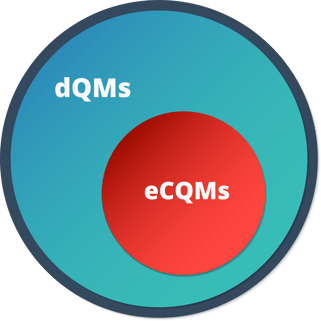
Most people are by now familiar with electronic clinical quality measures (eCQMs), which were originally introduced in the CMS Meaningful Use program. A universally accepted definition of dQMs is still under development, but they are considered to be an expansion of the eCQM concept in both data sources and scope of measurement. While both eCQMs and dQMs are expected to use the same digital data and interoperability standards, eCQMs are generally more closely aligned with EHR data. dQMs, on the other hand, could use standardized digital data from many sources, including claims and patient-generated health data. In other words, eCQMs are a subset of dQMs; all eCQMs are dQMs, but not all dQMs are eCQMs.
CMS set 2025 as its target date to transition to entirely digital quality measures reporting. The agency also solicited stakeholder feedback in its most recent inpatient proposed rule. Some of the key elements under consideration are listed below.
Expanding data sets and data sources
As mentioned above, dQM expands the use of data sources and their aggregation beyond the EHR or administrative data sets. This includes payer claims, case management, registries, HIEs and patient-generated health data, including patient-reported outcomes (PROMs).
FHIR-based APIs are the preferred interoperability standard to exchange standardized data elements, including social determinants of health.
Also See: FHIR for the Busy Quality Manager
Think of all the new quality measures that measure developers could create if they could integrate clinical and financial data and then generate and report the measures automatically to payers and providers. That could be particularly useful as the industry continues its shift to value-based care models and value-based reimbursement schemes.
Another example of how a dQM concept can expand quality measurement is technology itself. Data to create quality measures doesn't only come from EHR systems or claims databases. Today, clinical and financial data comes from a myriad of wearable health devices, smartphone apps, remote home monitoring tools, patient portals and more. Data to generate new dQMs can come from all those nontraditional technology sources—all without human intervention, so long as the data is compliant with the FHIR standard.
Two hurdles to implementation by 2025
Even though this is an aggressive timeline, it is certainly achievable given that eCQMs have been around for more than a decade. That said, CMS will have to solve two big challenges before a viable dQM system can be put into production.
The first is widespread standards-based interoperability between all the dQM data sources, including FHIR APIs and bulk FHIR. The second is the availability of high-quality standardized data that conforms to a common data standard. This is the mission of the Health Level Seven International Quality Improvement Core Implementation Guide, also known as HL7 QI-Core.
Overcoming these challenges could certainly pay rich dividends in improving the quality of patient care, all while advancing value-based payments and reducing provider burden.
The time to start thinking about dQMs and preparing for them is now. We'll be revisiting dQMs regularly on our Medisolv blog as CMS' digital quality measure initiative moves forward.
Learn more about how Medisolv's ENCOR quality reporting software platform can help your hospital or health system prepare for dQMs.
Stay Ahead of the Quality CurveMedisolv Can Help
Here are some resources to help you get started:
|





Comments