What is Social Determinants of Health (SDOH) Data?

The Covid pandemic not only uncovered significant data gaps in our public health system but also identified a need to better understand the intersection of how social determinants of health impacts patient outcomes. Both HHS and CMS have recently indicated they will pursue strategies to address this head on in their various programs. Stratification of quality and safety measure results and better collection of Social Determinants of Health (SDOH) data by providers at the point of care are their priorities.
Social Determinants of Health (SDOH) Data: The Key to Health Equity?
The debate over how we as a nation of health care providers, patient advocates, and policymakers can collectively achieve health equity for all, one thing has become increasingly clear: data, in particular social determinants of health (SDOH) data, will play a powerful role in our march towards progress. SDOH data has the potential to be the Rosetta Stone for establishing benchmarks, tracking progress, and identifying the gaps, biases, and disparities that have gone unchecked for too long.
And, as with all things data related, it will inevitably be up to quality improvement leaders like you to lead the way. But what does that mean for your quality improvement team and your healthcare system now? Here are some initial thoughts to help you prepare for the essential—but still evolving—journey ahead.
What is SDOH data?
The U.S. Department of Health & Human Services (HHS) defines social determinants of health (SDOH) as “the conditions in the environments where people are born, live, learn, work, play, worship, and age that affect a wide range of health, functioning, and quality-of-life outcomes and risks.” SDOH data, therefore, is intended to track those “conditions.” HHS currently groups SDOH into 5 categories:
- Economic stability > A patient’s financial resources, including income, employment, housing stability, and food security
- Education access & quality > A patient’s ability to access and advance their lives through education, from early childhood to higher education
- Healthcare access & quality > A patient’s access to and understanding of health care, including primary care access, insurance coverage, and health literacy
- Neighborhood and built environment > The quality of where a patient lives, including air and water quality, crime rates, access to healthy food, and more
- Social and community context > A patient’s relationships with friends, family, co-workers, and the community, which can be impacted by issues like discrimination, abuse, and incarceration
SDOH often intersect with our broader determinants of health. Gender, for example, may play a role in a patient’s educational opportunities, income level, or vulnerability to abuse.
While SDOH may not be medical in nature, the impact that they can have on a patient’s wellbeing and ability to follow their treatment plans is profound. If we ignore them, we’re simply not doing our job as healthcare providers.
Look for new ground rules of SDOH data to emerge.
CMS has for many years collected Race and Ethnicity data as “supplemental” to quality reporting, so it should come as no surprise that CMS has indicated that additional SDOH data will be an important element in quality measures and payment programs going forward.
CMS is engaged with standardization bodies like HL7 to develop universal standards that ensure healthcare systems across the country are collecting the right SDOH data in the right ways, consistently and accurately. There are some historical frameworks for standardizing SDOH data, but those were built for very specific applications, such as HIV surveillance and disaster recovery. What we now need is an SDOH framework specifically designed with quality measures in mind.
Z codes: An early solution?
One possible solution for the standardization of SDOH data are Z codes, the ICD-10-CM encounter reason codes developed to document SDOH data. There are currently nine Z code groups related to SDOH:
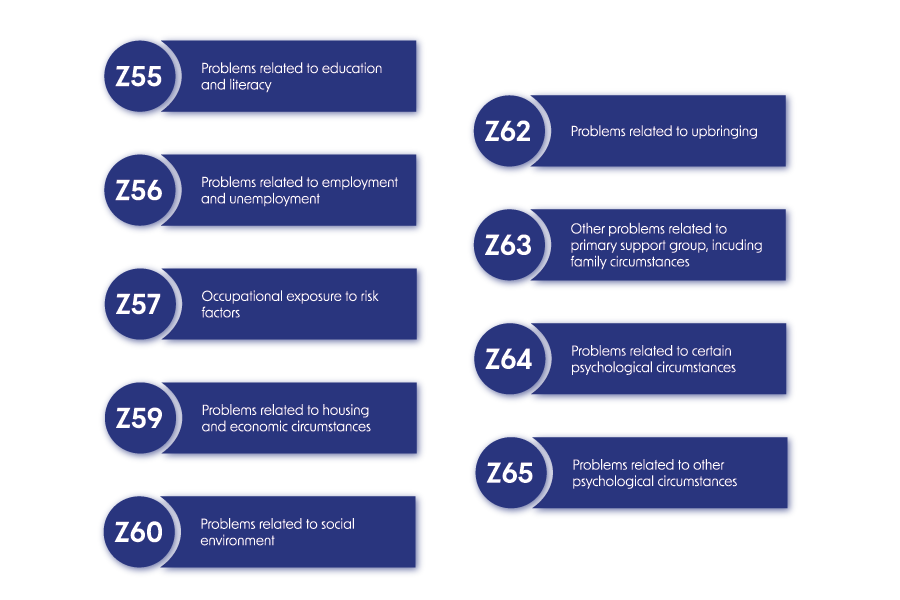
Z codes are still a significantly underutilized tool, and the degree to which they’re captured—and captured correctly—varies greatly from provider to provider. When comparing Z code data across institutions it’s still too soon to know if we’re comparing differences in the actual data, or differences in how the data was collected. Process metrics around how Z code data is collected could be on the horizon. Z-Codes are also included in the Gravity project within the HL7 FHIR standards for widespread digital interoperability.
That being said, if you’re not already using Z codes, you owe it to yourself, your patients, and your healthcare system to consider them. CMS has issued a helpful (and surprisingly easy to understand!) infographic that outlines the steps you and your team can take to make them part of your quality improvement initiatives now.
Think beyond Z codes.
Are Z codes the final answer on SDOH data? Maybe. But this is also a unique opportunity for our healthcare industry to innovate, because the data we need to collect goes so far beyond traditional healthcare data.
Consider, for example, how the financial services industry collects and uses customers’ income and employment data to deliver targeted products and services on an individual level. What can we learn from industries outside our own to build new data models that enable us to create a more equitable system of patient-centered care?
Or perhaps the solution isn’t that complicated at all. In a recent HIMSS panel that I participated in, my fellow panelist, Geoff Dougherty, Ph.D., Deputy Director of Population Health for the state of Maryland’s Health Services Cost Review Commission, suggested that a lot can be gleaned from three critical pieces of information: education level, employment, and income. Perhaps a simpler solution would make SDOH data simultaneously more reliable and more useful in our ability to deliver equitable, whole-person care.
Start understanding your SDOH data now.
So, the moral of the story is that we still have a lot of heavy lifting to do in order to understand, standardize, collect and make meaningful use of SDOH data. But one thing’s for sure: it’s coming. You can wait until CMS makes SDOH data mandatory (which, it’s safe to assume, will happen). Or you can do what we always recommend here at Medisolv: take the time to start understanding your data now. As mentioned, Z codes are a great place to start. There are also a growing number of SDOH screening tools available, both analog and electronic, that you can research and integrate into your data collection processes at the point of care now.
Beyond the looming regulatory future, SDOH data will be invaluable to your ultimate mission, which is to improve patient care. It can give you a clearer understanding of your patient mix and help spot disparities in outcomes that you can then rectify through adjustments in process of care. SDOH data could also give you the power to start managing a patient’s care on an almost predictive level. Consider how often social factors, such as a patient’s ability to afford medications or access to transportation, impede their “normal” care pathway. The more we can identify these risk factors early on, the more we can put targeted interventions in place to shape better outcomes.
Early adopters (like you!) should be incentivized.
As you begin to roll up your sleeves on this topic, my hope is that regulatory bodies will consider how to reward healthcare systems like yours—the ones who are not afraid to dive into the murky waters of SDOH data now.
As a national leader in healthcare payment reform, Maryland’s all-payer model is built around incentivizing health systems for both improvement and attainment around a variety of quality, safety, and satisfaction measures. The state has taken the first step to incentivize health equity improvements by including SDOH data in its Readmission Reduction program. An improvement-only based incentivization program could help healthcare systems get comfortable with SDOH data and measurements now, so that we can achieve our health equity goals sooner rather than later.
Let’s Work Together to Achieve Health Equity Now
Contact us today to learn how you can begin to monitor your quality data through a health equity lens. Or explore our library for more insights:
Medisolv Can HelpAlong with award-winning software, each client receives a dedicated Clinical Quality Advisor that helps you with your technical and clinical needs. We consistently hear from our clients that the biggest differentiator between Medisolv and other vendors is the level of one-of-one support. Especially if you use an EHR vendor right now, you’ll notice a huge difference.
|






Comments