MIPS 2018: Fact or Fiction?
By Denise Scott, M.M. RN-BC August 31, 2018 Regulatory Updates: Ambulatory

Will the real MIPS please stand up? Trying to get your facts straight for MIPS reporting can be confusing and frustrating. And with a positive or negative payment adjustment at stake, having the right information is crucial for achieving MIPS success.
So, what’s the truth about MIPS round two? Are you up to speed with accurate requirements and changes for 2018?
Set your uncertainties, questions and worries aside. Today, we’re dispelling the biggest misconceptions about MIPS reporting in 2018 with nine hard facts.
1. ALL FOUR MIPS CATEGORIES WILL COUNT TOWARD YOUR FINAL SCORE IN 2018.
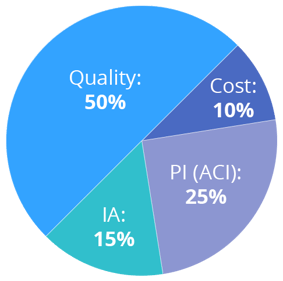
Unlike 2017, there are four categories that will count toward your overall MIPS score in 2018: Quality, Improvement Activities (IA), Promoting Interoperability (PI, formerly Advancing Care Information) and new this year, Cost.
Since Cost will now be a part of final MIPS score calculations, the percentage for the Quality category decreased from 60% to 50%.
Fact: Your performance in four categories will make up your final MIPS score in 2018. |
2. PERFORMANCE DOESN'T COUNT IN THE COST CATEGORY.
Since your Cost score is calculated through the administrative claims that you submit, no action is required for the Cost category. But don’t let this fool you, because performance still matters.
CMS will evaluate your Cost score based on the average of two measures—the Medicare Spending per Beneficiary (MSPB) and the Total Per Capita Costs for All Attributed Beneficiaries (TPCC) measures—during a 365-day period. Your performance in these measures will be compared with other MIPS Eligible Clinicians and groups in 2018.
You can review a final report of your 2017 Cost points on the Quality Payment Program (QPP) portal. This will help you access your 2017 performance and identify areas of improvement for 2018. Here’s an example of a 2017 final MIPS report for the Cost category:
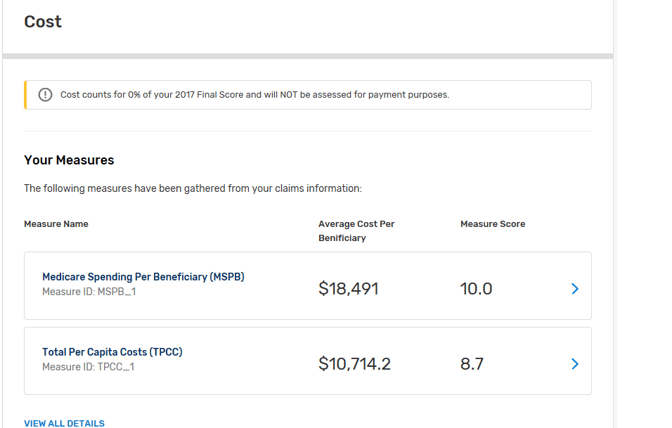
The QPP final MIPS report will provide a breakdown of your final scores for the Quality, IA and PI categories as well.
Fact: Performance matters in all four categories of MIPS 2018 including the Cost category. |
3. YOU HAVE THE OPTION OF REPORTING VIA A VIRTUAL GROUP.

In addition to reporting as an individual or as a group, you may report as a Virtual Group for year two of MIPS. The deadline to let CMS know was December 31, 2017.
A Virtual Group is made up of two or more individual or group eligible clinicians who choose to submit their MIPS data virtually under a single TIN. That means that clinicians do not need to be in the same area of the country or in a similar specialty, but they have to align themselves as a group. (it’s kinda like pen pals…with you know, money on the line).
If you plan on reporting as a Virtual Group in 2019, you need to let CMS know by December 31, 2018 and be ready to go on January 1, 2019.
Fact: For 2018 MIPS reporting, you can report as an individual, a group or as a virtual group |
4. THE 2015 CEHRT BONUS APPLIES TO ALL FOUR MIPS CATEGORIES.

You can submit your MIPS data using the 2014 or 2015 edition of CEHRT—but keep in mind that Eligible Clinicians who use the 2015 edition of CEHRT for MIPS reporting can receive a 10-point bonus.
However, this bonus is only applicable for reporting measures in the PI category for 90 days using 2015 CEHRT. It does not apply to the other categories.
.gif?width=300&name=giphy%20(9).gif)
Fact: You can earn a 10-point bonus for using the 2015 edition of CEHRT to report your MIPS measures in the Promoting Interoperability category. |
5. ELIGIBLE CLINICIANS MUST ONLY REPORT SIX QUALITY MEASURES.

The reporting requirements for the Quality category will remain the same for 2018. You must still report a total of six Quality measures, and it’s important to choose your six best performing Quality measures for optimal results.
Remember, reporting more than six Quality measures will not get you extra points. Instead, CMS will simply choose which Quality measures to count toward the final MIPS score on your behalf.
Fact: You must report no more and no less than six Quality measures. Be sure to include an Outcome measure as one of your six Quality measures. A high priority measure can be submitted only if an outcome measure is not available. |
6. YOU CAN REPORT YOUR DATA USING MULTIPLE REPORTING METHODS.

Eligible Clinicians are required to choose one reporting method for each MIPS category. Take a look at the reporting options below:
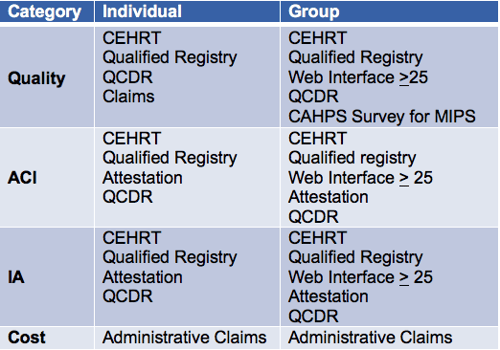
According to the 2019 QPP proposed rule, Eligible Clinicians may be able to choose more than one reporting method in 2019. CMS would determine a score using the data submission with the greatest number of measure achievement points. You can find out if this proposed change will be finalized in the final rule, which will be published this fall.
Fact: While there are several reporting options for each MIPS category, Eligible Clinicians can only choose one. |
7. DATA COMPLETENESS FOR THE QUALITY CATEGORY HAS INCREASED.

To successfully fulfill the reporting requirements for the Quality category, you’ll need to meet the Case Minimum requirement of 20 cases for 2018.
In addition, you must include at least 60% of all patients eligible for the measure across all payers. This number has increased from 50% in 2017.
Even if you perform well in the Quality category, you’ll only receive one point for each measure if you don’t meet the Data Completeness requirement. CMS will only make exceptions for small practices.
Fact: Measures must contain at least 60% of all Eligible Clinician patients across all payers in 2018. |
8. YOU DON'T NEED TO LET CMS KNOW IF YOU CHOOSE TO SUBMIT YOUR DATA USING THE CMS WEB INTERFACE.

Groups with more than 25 Eligible Clinicians have the option of submitting their measures using the CMS Web Interface.
If you plan on reporting your MIPS data through the CMS Web Interface, you had to have let CMS know by June 30th of this year. Otherwise, you’ll need to choose a different reporting method for 2018.
Fact: Groups who plan on submitting their MIPS data using the CMS Web Interface had to have let CMS know by June 30, 2018. |
9. THERE IS NO PICK YOUR PACE REPORTING OPTION IN 2018.

Well, sort of. To avoid a penalty in 2018, you must submit MIPS measures that total at least 15 MIPS points from one category, or a combination of categories. Any amount of reporting worth over 15 points determines the amount your fee schedule will increase in 2020, so seek your highest level of performance as a goal.
You’ll receive a negative reduction of up to -5% for not reporting or not reporting at least enough data to earn 15 MIPS points, and a positive adjustment of up to +5% based on your performance across all categories in comparison to your peers.
Fact: To avoid a penalty in 2018, you'll need to earn at least 15 points. |
DO YOUR RESEARCH
Successfully fulfilling your MIPS requirements begins with research, research and a little more research. Here are some additional resources to help you prepare for MIPS 2018:






Add a comment