How to Implement the Hybrid Mortality Measure

A new hybrid measure is on the horizon. Yes, another new measure that will be required for successful completion of your IQR program requirements. Here’s everything you need to know.
Let’s start with the basic information about hybrid measures. If you know this part, skip ahead.
A hybrid measure combines claims data and electronic data from your EHR; thus, creating a hybrid measure.
To be successful at capturing the hybrid measures you need to be successful at capturing both of those key data sources.
Claims data you’ve been doing for a long time (submitted to bill insurance companies for the patients’ visits). No big deal. The key here is that the claims data must be linked with all the EHR data (all of the data captured electronically during a patient’s visit).
Why do we need hybrid measures?
Here’s a summary of the reasons CMS is moving toward hybrid measures.
Preference: Clinicians have been talking about this for years. They believe that using clinical data to assess how sick a hospital’s patients were at the time they came into the hospital, is a more accurate depiction of their challenges, rather than just straight billing.
Data collection: That transition from paper to EHR creates an opportunity to integrate clinical information into hospital quality measurement without the burden of manual chart abstraction.
Accuracy: This is a biggie. The data we get from claims does not contain any risk factors associated with severity, which can really impact these calculations. The best-performing risk adjustment models typically include risk factors that assess both comorbidities and severity. Historically, the claims-based models do assess the comorbidities, but the electronic clinical data provides the measure of severity when the patient is admitted.
What is the Hybrid Hospital-Wide All-Cause Risk Standardized Mortality measure?
- Full Name: Hospital-Wide All-Cause Risk Standardized Mortality measure
- Measure ID: CMS 844
- Short Measure Name: HWM
- Voluntary reporting period: July 1, 2022 - June 30, 2023
- Mandatory reporting period: July 1, 2023 – June 30, 2024
- Publicly reported with 30-day review period prior to public reporting
How does CMS calculate the Hybrid Mortality Measure?
This measure calculates a hospital’s hospital-wide mortality rate. The calculation is complicated to explain. It incorporates a lot of different things to provide hospitals with their performance.
The rate is calculated by:
- Using all-cause mortality hospital rates
- Combining claims and EHR data
- Adjusting for differences in case mix and service mix across all hospitals
The goal in this is:
- To identify the critically ill patients that have a higher probability of mortality and take that into account when calculating this rate.
How and when do we submit the Hybrid Mortality Measure?
By 2023 the hybrid mortality measure will be required as a part of your IQR requirements. There is one year of voluntary submission proceeding that requirement and it start in July of this year.
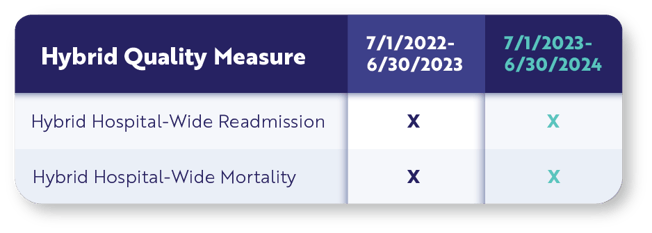
Hospitals must submit certain data elements from a patient’s electronic record and submit to CMS using a QRDA file.
Sound familiar? It’s very similar to what you do for eCQM submissions right now. In fact, there is a specification for this measure, and it looks like an eCQM spec. The logic is in the same format but it’s not technically a measure specification. Think of it more as a guide.
What is needed to capture the Hybrid Mortality Measure?
You need one more acronym definition here to understand this measure. CCDE stands for Core Clinical Data Element. These are the items you need to map in your EHR and include in your QRDA file to CMS.
Let’s look at what you need from your EHR and from your claims data.
What EHR data is used?
The 10 CCDE that you must submit in the QRDA file are in two buckets: vital signs and lab results.
Vital Signs:
- Heart rate
- Systolic blood pressure
- Temperature
- Oxygen saturation
Lab Results:
- Hematocrit
- Platelets
- White blood cell count
- Sodium
- Bicarbonate
- Creatinine
What claims data is used?
These linking variables need to be included in the QRDA file that you submit to CMS. If they can’t connect the two then CMS won’t be able to calculate the measure.
Linking Variables:
- CMS certification number
- Health Insurance Claim Number or Medicare Beneficiary Identifier
- Date of birth
- Sex
- Admission date
- Discharge date
Implementing the Hybrid Mortality Measure
Alright, I think you’re probably ready for the explanation now.
Download this and keep it at your fingertips. Clients: You have this available in the product when you click on the Hybrid Measures tab.
The spec can look completely overwhelming when you first look at it. But it’s not that difficult to understand once you know what you’re looking at.
Identifying the population
The Initial Population is all inpatients that are 65 or older and up to 94 years of age who have Medicare as their payer and a stay of less than 365 days.

Patients will be excluded if they have inconsistent or unknown vital status, are discharged against medical advice, or if they are admitted for crush injury, burn, intracranial injury, skull and face fractures, open wounds of head, neck, and trunk, or spinal cord injury.
Understanding the logic
Alright, now let’s move onto the logic section.
Results

This is telling you that it’s looking for the earliest instance of at least one of the 10 core clinical data elements within specific time frames.
Functions
Below is a picture of the “Functions” part of the specification which tells you the specific timing of the CCDE.

In a nutshell, this measure will capture the first instance of documentation.
This means the earliest instance of documentation that meets the timing requirements above will be evaluated and included in the QRDA file.
^^This is key.
The measure will look back to find these CCDE 24 hours before the patient becomes an inpatient. It will also look for any labs and weights captured 24 hours after admission as an inpatient. And it will also look for vital signs captured two hours after admission.
Put simply, you’ve got to capture all 10 CCDE within these narrow time frames or it will not be included in the QRDA file you send to CMS. And remember, those CCDE are telling CMS how sick your patients are and adjusting your mortality rate based on that information.
Data Elements
Alright, remember when we looked at which core clinical data elements are used from your EHR at the top of this article? That is what you are seeing listed here in the data elements portion of the specification.

The data elements listed here are the ones you must map in your EHR to properly capture the measure. To the right of each of these elements is a long string of numbers. This is the OID (Object Identifier Code). This is the number you put into the Value Set Authority Center website to look up the value sets to map to your system.
Clients: you can just use the value set search tool in our software.
Implementation Process
Essentially, you must take all the data elements listed in the specification and map the value set codes to the places you document those elements in your EHR system.
Below I’ve mapped out the hybrid mortality measure workflow and I think it simplifies what you need to do here.
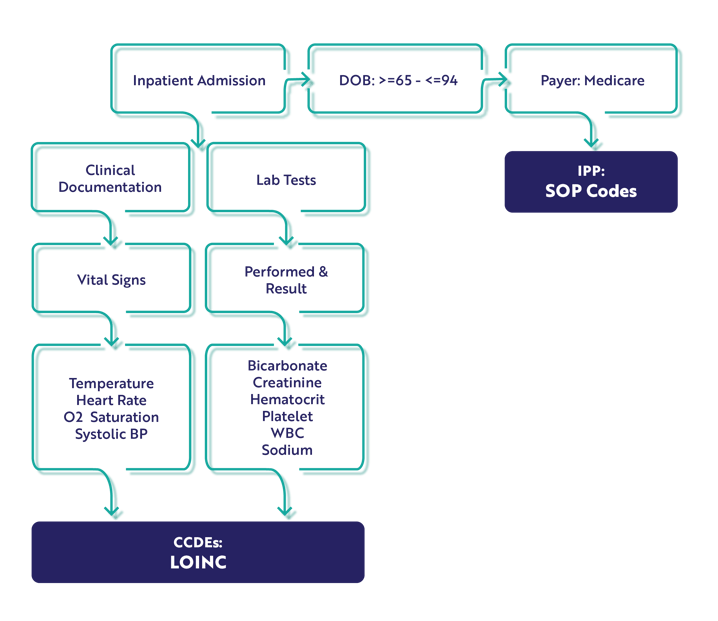
Mapping the Hybrid Mortality Measure
Ask yourself, where are you documenting all these elements in your EHR? This list you create contains all the places where these CCDE are captured. This is also your list of what needs mapped in your system.
Monitoring and improving your Hybrid Mortality Measure results
Once you think you’ve got this all set up and implemented, then comes the real test. You must have a way of going into your system and reviewing to see if you are really getting all the elements captured.
The tough part about this measure is that you won’t know your performance until CMS compiles the whole thing for you. But you sure as heck know that you don’t want to have a lower score because of something stupid like forgetting to map your blood pressure documentation.
Shameless Plug
At Medisolv we have a CCDE missing results page for our clients. This shows you what elements are missing before you get to the submission phase.
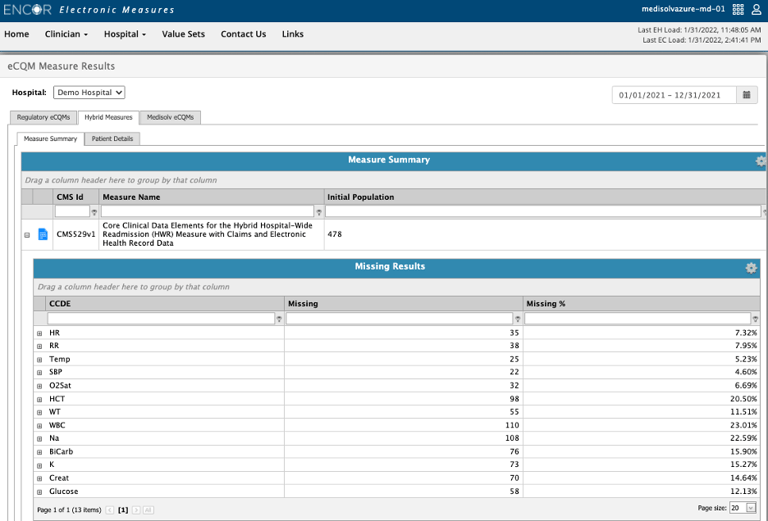
Even if you don’t use Medisolv, you should have a way of reviewing this data to ensure you aren’t making a mistake that is easily identified and fixed.
If you would like to learn more about the implementation of the hybrid mortality measure, you can watch our on-demand webinar CMS IQR Program: Required Electronic Measures. Resident eCQM expert, Kristen Beatson, dives deeper into the requirements of both hybrid measures.
Looking for someone to keep you updated on changing regulations?
Along with award-winning software, each client receives a dedicated Clinical Quality Advisor that helps you with your technical and clinical needs. We consistently hear from our clients that the biggest differentiator between Medisolv and other vendors is the level of one-of-one support. Especially if you use an EHR vendor right now, you’ll notice a huge difference.
Here are some resources you might find helpful: |





Comments