MSSP ACO QPP 2023 Requirements

The Quality Payment Program (QPP) has allowed large organizations to use the CMS Web Interface reporting method to complete MIPS requirements since the program launched in 2017. This gave these organizations the option to report a sampling of 248 patients (selected by Medicare Part B claims) across all their practices. CMS will completely sunset the CMS Web Interface reporting option by 2025.
In 2025, all MSSP ACOs must report either eCQMs or CQMs for all patients, all payers, across all practices for 365 days of the year.
Figuring out data aggregation, de-duplication, and comprehensive performance review before 2025 is the key to your success. Below is a summary of your requirements and tips for getting started.
APM Performance Pathway (APP) Reporting Requirements
There are three reporting frameworks available in the Quality Payment Program, but MSSP ACOs can only submit to one, the APM Performance Pathway (APP) reporting framework.
Also read: A comparison of the 2023 requirements for all three reporting frameworks.
APP Framework Category Weights
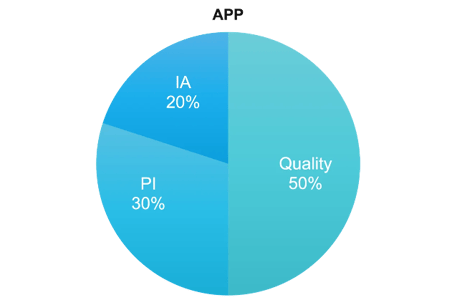
For the APP framework there are three categories, Quality, Promoting Interoperability, and Improvement Activities. Cost is weighted at 0%. This article will focus on the Quality category only. See article above for information on the other categories.
Defining QPP Collection Types
Collection types are the way you report the data to CMS. You can think of them like measures. There are six collection types in 2023.
- eCQMs (Electronic Clinical Quality Measures)
- MIPS CQMs (previously called Registry measures)
- QCDR measures (Qualified Clinical Data Registry)
- Medicare Part B Claims measures
- CAHPS for MIPS survey
- CMS Web Interface measures (<< not available in 2025)
NOTE: CMS has added a new collection type for 2024. Learn more about the Medicare CQM >>
APP Framework: 2023 Quality Category Requirements
Category weight: 50% of total QPP score
Performance Period: 365 days
Requirements:
Option 1 (<<your only option in 2025)
- Submit 3 eCQMs or CQMs
- You may use a combo of collection types (eCQMs or CQMs)
- Two administrative claims measures are calculated automatically by CMS
- CAHPS for MIPS survey
Option 2 (<<not available in 2025)
- Submit 10 CMS Web Interface measures
- Two administrative claims measures are calculated automatically by CMS
- CAHPS for MIPS survey
Option 3 (<<not available in 2025)
- Submit 3 eCQMs or CQMs AND 10 CMS Web Interface measures
- You may use a combo of collection types (eCQMs or CQMs)
- CMS will give you the highest score out of the two options when you submit both
- Two administrative claims measures are calculated automatically by CMS
- CAHPS for MIPS survey
Measure list:
Quality Measures
- eCQMs/CQMs
- Quality ID: 001 Diabetes: Hemoglobin A1c (HbA1c) Poor Control
- Quality ID: 134 Preventive Care and Screening: Screening for Depression and Follow-up Plan
- Quality ID: 236 Controlling High Blood Pressure
- CMS Web Interface Measures
- Quality ID: 001 Diabetes: Hemoglobin A1c (HbA1c) Poor Control
- Quality ID: 134 Preventive Care and Screening: Screening for Depression and Follow-up Plan
- Quality ID: 236 Controlling High Blood Pressure
- Quality ID: 318 Falls: Screening for Future Fall Risk
- Quality ID: 110 Preventive Care and Screening: Influenza Immunization
- Quality ID: 226 Preventive Care and Screening: Tobacco Use: Screening and Cessation Intervention
- Quality ID: 113 Colorectal Cancer Screening
- Quality ID: 112 Breast Cancer Screening
- Quality ID: 438 Statin Therapy for the Prevention and Treatment of Cardiovascular Disease
- Quality ID: 370 Depression Remission at Twelve Months
Claims Measures
- Hospital-Wide, 30-Day, All-Cause Unplanned Readmission (HWR) Rate for MIPS Eligible Groups.
- Clinician and Clinician Group Risk-standardized Hospital Admission Rates for Patients with Multiple Chronic Conditions
CAHPS for MIPS Survey measure
Achieving Shared Savings in 2023
In 2023, for an MSSP ACO to get the maximum shared savings they must achieve a quality performance score that is greater than or equal a certain percentile of the benchmark and meet the Shared Savings Program Quality Performance Standard. CMS has implemented a sliding scale to give ACOs some percentage of the Shared Savings (not max) if they don’t meet the Quality Performance Standard but do achieve a quality performance score.
Option 1
- Report all 3 eCQMs/CQMs, meet the data completeness requirement (70%) and the case minimum requirement for each measure.
- Achieve a quality performance score = > 10th percentile of the performance benchmark on at least 1 outcome measure.
- Achieve a performance score that is = > 30th percentile on at least 1 of the remaining measures.
These are very low performance rates. You are likely achieving above these percentages for your CMS Web Interface measures. Here is an excel sheet that shows you the deciles for these measures. 10thpercentile means decile 1 in the sheet. 30th percentile means decile 3 in the sheet. Both Diabetes and Controlling High Blood Pressure are outcomes measures. If you achieve either of these scores below, you’d be eligible to share in saving.
- Option 1 Scores to Achieve Shared Savings
- (Decile 1) 99.52 - 93.34 on Diabetes: Hemoglobin A1c (HbA1c) Poor Control (>9%) <<INVERSE MEASURE
- (Decile 3) 51.36 - 56.60 on Controlling High Blood Pressure
- 0.7% or higher on Preventive Care and Screening: Screening for Depression and Follow-Up Plan
- Option 2 Scores to Achieve Shared Savings
- (Decile 3) 75.00 - 57.61 on Diabetes: Hemoglobin A1c (HbA1c) Poor Control (>9%) <<INVERSE MEASURE
- (Decile 1) 2.74 - 41.95 on Controlling High Blood Pressure
- 0.7% or higher on Preventive Care and Screening: Screening for Depression and Follow-Up Plan
Option 2
- Report all 10 CMS Web Interface measures
- Achieve a quality performance score that is = > 30th percentile across all MIPS Quality performance category scores (excluding facility-based scoring)
NOTE: In 2024, this goes up to = > 40th percentile for CMS Web Interface measures. But even more importantly (!) this remains at = > 40th percentile in 2025 which means your eCQMs/CQMs must reach decile 4 by 2025.
One final thing to know about the Shared Savings portion. You will know individual measure performance benchmark score ranges (reference the excel sheet I gave you). You will not know the Quality Performance Standard threshold which is determined by looking at all MIPS Quality Performance Scores nationwide. CMS calculates that after the submission is done (March 2024).
Data Completeness Requirements
There has been SO MUCH discussion on this topic. I once watched an ACO representative grill a CMS representative in a live panel discussion for no less than 20 mins on this topic. I think we all left even more confused. CMS attempted to make it clearer (which they are terrible at). So, here’s the best summary and documentation I can offer you.
An ACO must submit their entire “universe” of patients. None of your practices can be excluded based on populations. The data completeness threshold really would only be applicable in a MIPS CQM situation and even in that situation you still must have the entire universe of practices/patients and only achieve 70% completeness on the denominator patients.
Take a look at pages six and eight of the APP guidance document here.
eCQM Data Completeness Criteria Summary
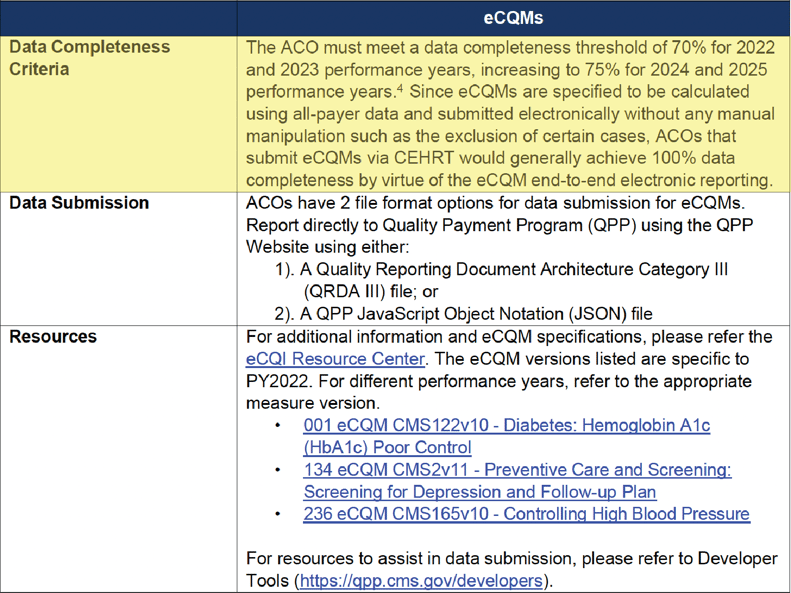

MIPS CQM Data Completeness Criteria Summary
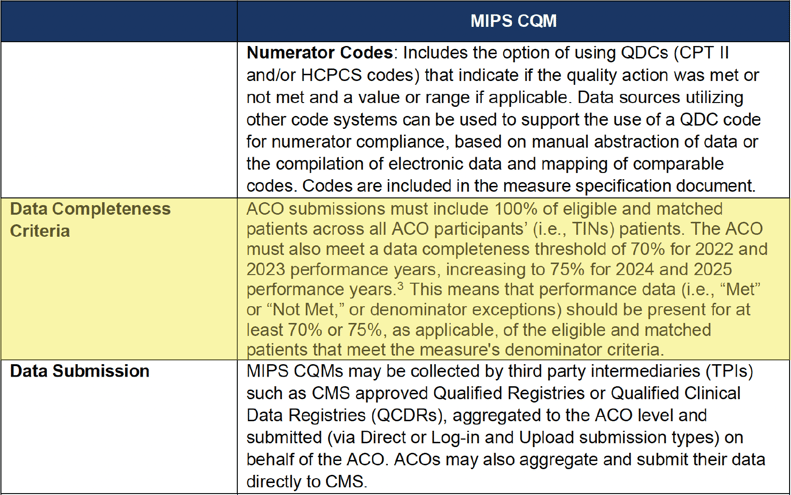
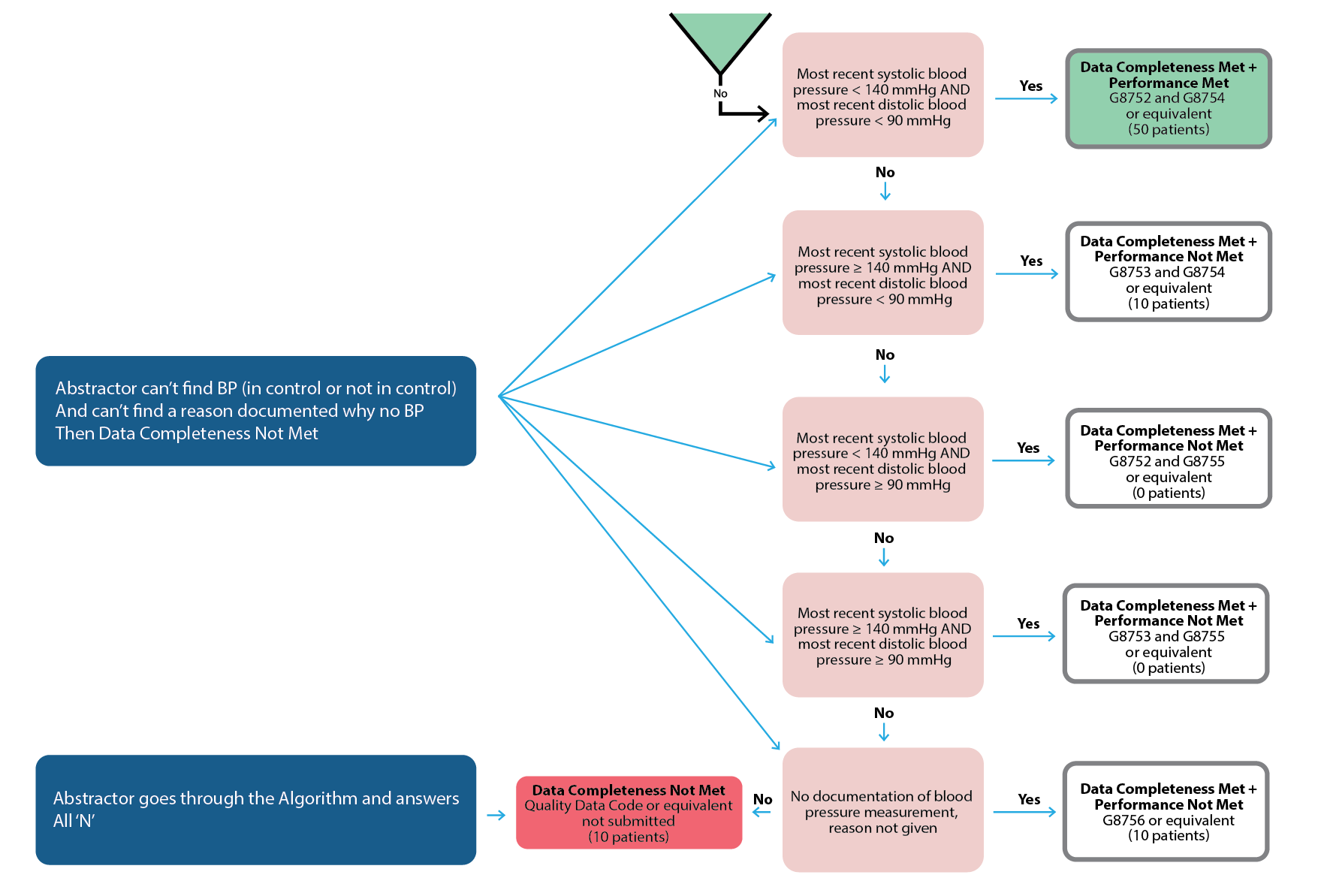
When is the data completeness threshold applicable?
It’s an unlikely scenario. But in some cases, an abstractor can't find the documentation that’s required by the measure. In this red scenario below an abstractor answers “no” to algorithm questions for more than 30% of cases.
How to Get Started With eCQM/CQM Reporting
ACOs must learn to juggle multiple, disparate EHRs and data collection methodologies. Developing a cohesive data aggregation system is going to be a major undertaking. Your senior leadership, quality management, and information technology teams need to start planning what that looks like for your ACO now.
The most important thing you can do right now is understand what your data landscape looks like. Here are a couple of questions you should know.
- Which practices are on which EMRs? Make a list.
- How many instances of each EMR vendor do you have?
- Do you have any practices still on paper charts? (<<If so, you cannot report to CMS.)
- How many practices are on less common EMRs?
- Can every single practice generate a QRDA I file (<<Applicable for eCQMs. Especially focus on those practices with less common EMRs.)
- Do you capture CPT II (G codes) in a database for all practices? (<<Applicable for MIPS CQMs.)
This information will help you to choose whether you want to submit eCQMs or MIPS CQMs. It will also inform you as to whether or not you have to set up conversations with any practices not able to provide your group with what you need.
How Long Will the Data Acquisition Process Take?
This is completely dependent upon your organization set up. For most of our clients, we tell them to estimate a 6–8-month implementation time before you start to see any meaningful data.
Final Thoughts: Don’t Wait
Yes, it’s true. History has proven that CMS could change the rules and deadlines on us any minute, however, in the 2023 final rule CMS made it clear that they are still intending to sunset the CMS Web Interface Measures by 2025 for everyone.
It's in your best interest to start looking at your data through the all-patients, all-payers, all-practices lens now. It is the key to unlocking so many other patient care goals for you, including improving population health, reducing health care costs, and advancing health equity. For too long, the CMS Web Interface had made quality reporting a box that organizations had to check. It’s time now for organizations like yours to lead the charge to elevate the role of quality data in patient care. Together, we have the power to put quality data to good use.
More Resources to Prepare Your ACO For What’s Next
At Medisolv, we offer so much more than quality software and start-to-finish submissions management. We’re the quality improvement partner committed to deciphering and anticipating CMS’s regulatory changes for you—so that you can keep your organization ahead of the curve.
Check out some of our additional resources now:
- eBook: CMS Web Interface Transition Guide
- Article: 2023 QPP Requirements
- On-Demand Webinar: Preparing your ACO for APP Reporting
Medisolv Can HelpAlong with award-winning software, each client receives a dedicated Clinical Quality Advisor that helps you with your technical and clinical needs. We consistently hear from our clients that the biggest differentiator between Medisolv and other vendors is the level of one-of-one support. Especially if you use an EHR vendor right now, you’ll notice a huge difference.
|



.png?width=352&name=2026%20Quality%20Reporting%20Deadlines%20Guide%20(1).png)


Comments