STEMI: The First eCQM for the OQR Program

For over a decade CMS has been incorporating Electronic Clinical Quality Measures (eCQMs) into the Inpatient Quality Reporting (IQR) program. For the first time, CMS has released an eCQM for the Outpatient Quality Reporting (OQR) program. This new measure (STEMI OP-40) is required for successful completion of your OQR program requirements in 2024. Hospitals may voluntarily report the measure in 2023.
What is the STEMI eCQM?
STEMI stands for ST-Segment Elevation Myocardial Infarction, a patient diagnosis that leads to increased mortality and morbidity. Nearly two lives per 1,000 patients are lost per hour of delayed treatment.2
This measure is not technically new. You’ve been measuring a version of this measure on the chart-abstracted side for a while now. OP-2 (Fibrinolytic Therapy Received Within 30 Minutes of ED Arrival) is a chart-abstracted measure required for submission in the OQR program.
In 2025, OP-2 will be removed from the OQR program. Effectively, the STEMI eCQM (mandatory in 2024) replaces the chart-abstracted measure.
The STEMI eCQM is focused on ED care. Its goal is to measure the number of ED patients properly cared for who had a diagnosis of STEMI. Proper care is defined as:
- Fibrinolytic therapy (within 30 minutes of arrival)
- OR Percutaneous Coronary Intervention (PCI) (within 90 minutes of arrival)
- OR Transfer (within 45 minutes of arrival)
Why Measure STEMI Treatment Electronically?
This measure has been an area of focus for decades and multiple studies over that time have shown that timely action leads to better outcomes for patients.
Unsurprisingly, the progress hospitals made on this measure was hit hard recently because of the COVID-19 pandemic. One study showed an ~8 fold increase in hospital mortality for STEMI patients in 2021. So, the work we must do to improve this measure performance must continue.
Making this measure an eCQM ties in with CMS’ goal to go all digital by 2025. Could we expect more abstracted measures to switch to eCQMs?
A Review of the eCQM Specification
You can review the eCQM specification (located here) and get familiar with what you will need to map but here is the high-level summary to get you started.
Initial Patient Population/Denominator
Layman’s description: To get into the Initial Patient Population (IPP) and Denominator the patient must be an ED patient who is 18 years of age or older and has a STEMI diagnosis.
Simplified logic: Initial Population / Denominator
- Emergency Department visit
- >= 18 years of age
- Diagnosis of ST-segment elevation myocardial infarction (STEMI)
For this measure, the Initial Patient Population and Denominator are the same so once you’ve got this group of patients defined, we want to see if any of them will be moved into the Exclusion population.
Exclusions
Layman’s description: Once patients enter the Denominator population, they may be put into the Exclusion population if they have any of the following documented:
- Mortality in ED
- Active or Recent Bleeding
- Ischemic Stroke
- Malignant Intracranial Neoplasm
- Cerebral Vascular Lesion
- Non-Penetrating Head Trauma
- Active Peptic Ulcer
- Pregnancy
- Allergic Reaction
- Endotracheal Intubation
- Anticoagulant Medications
- Dementia
- Major Surgical Procedure
- Neurological Impairment
- Mechanical Circulatory Assist
- Cardiopulmonary Arrest
- Aortic Dissection
And finally, of the remaining patients in the Denominator (who were not excluded), we consider whether they make it into the Numerator population.
Numerator
Layman’s description: Anyone in the Denominator population who was not excluded AND received fibrinolysis within 30 minutes, OR PCI within 90 minutes, OR were transferred within 45 minutes of ED visit.
Simplified logic: Numerator
- Fibrinolytic Therapy starts 30 minutes or less after the start of ED visit
- OR Percutaneous Coronary Intervention starts 90 minutes or less after the start of ED visit
- OR Transferred out of ED within 45 minutes or less of the start of the ED visit
There are no Numerator Exclusions or Denominator Exceptions for this measure. Your performance rate is then calculated using these populations. The higher your score the better.
Setting Up the STEMI Workflow
Once you’ve pulled apart the specification the next step is to do a current state analysis of where these items are being captured in your current EHR set up. I find that a workflow graphic like the one I’ve provided below is helpful as you do this process.
You’ll see (from left to right) I listed the different populations followed by the population criteria statement(s), then an educated guess for where that documentation may be found in your EHR and then the type of codes you’ll need to map to capture that element.
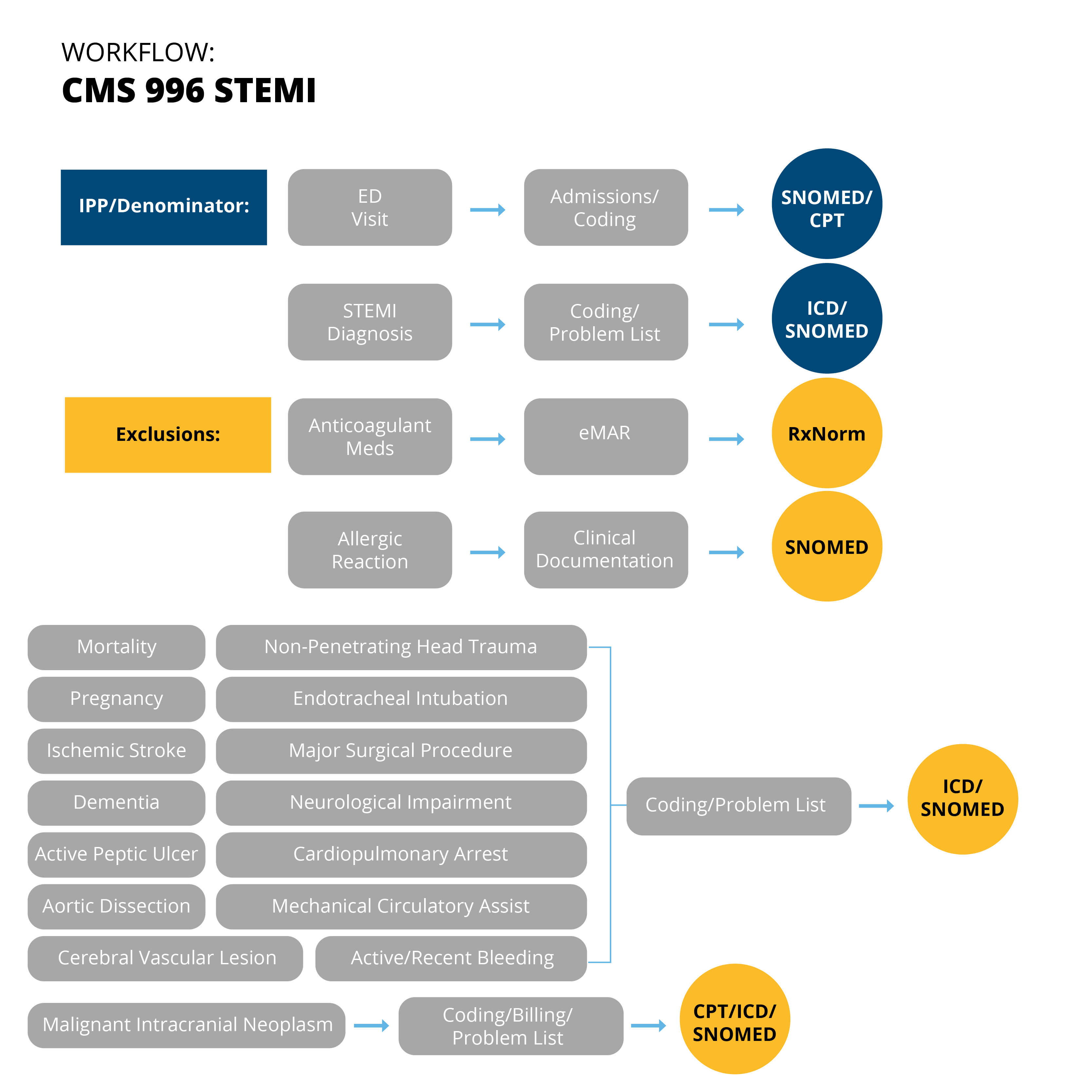
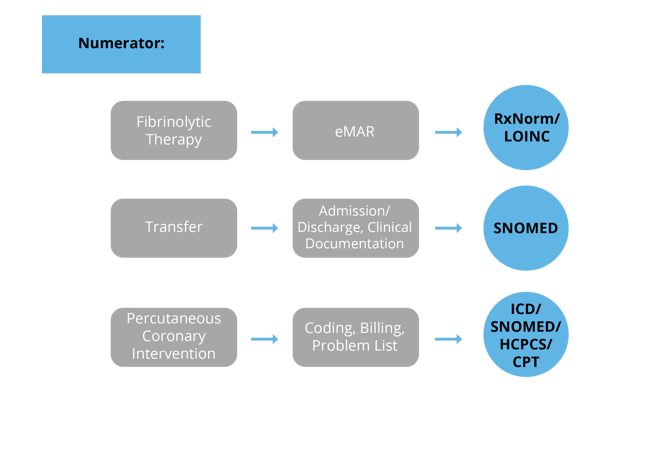
As you look at each population criteria statement fill in the information for your specific organization.
Do you capture this information?
- If not, what is the best way to capture the information going forward?
- If so, where do you currently capture this information?
- Will you need to make any changes to documentation processes?
- Are you capturing it in multiple places?
- If so, which documentation will give you the best results that are within the timing restrictions?
|
Learn how Medisolv can help you decipher this measure, and what we offer for it. |
Once Set Up, Validate
Once you have the measure set up in your system you can begin the validation process. Initially this process may take some time as you will be trying to resolve technical errors and problems with workflows, but after the kinks are worked out you can begin the real work of quality improvement.
Don’t go it alone! Reach out to us today to talk about how we can help your team. Medisolv plans on having the measure available to clients late this year or early next year (pending any other fatal logic flaws!). Leave all this measure deciphering to us. We will guide your team through measure set up, technical troubleshooting and error resolution, and come up with strategies for improvement like clinician adherence. Request a demo of our ENCOR for Electronic Hospital Measures software today.
Sources:
- https://ecqi.healthit.gov/ecqm/eh/oqr/2023/cms996v2
- https://ecqi.healthit.gov/sites/default/files/ecqm/measures/CMS996v2.html
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8515361/
- https://www.ncbi.nlm.nih.gov/books/NBK532281/
- https://www.ahajournals.org/doi/10.1161/CIRCULATIONAHA.117.032446
- https://www.ahajournals.org/doi/10.1161/JAHA.118.008096
- https://www.acc.org/latest-in-cardiology/articles/2021/09/21/12/05/stemi-management-update-2021
- https://www.sciencedirect.com/science/article/pii/S1936879814014411?via%3Dihub
- https://www.federalregister.gov/public-inspection/2021-24011/medicare-program-hospital-outpatient-prospective-payment-and-ambulatory-surgical-center-payment




.png?width=352&name=2026%20Quality%20Reporting%20Deadlines%20Guide%20(1).png)
Comments