Patient Safety: A Look Back at Health IT Evolvement

What is your hospital doing to develop and improve patient safety? Not sure where to begin? ECRI Institute recently released their list of the top 10 patient safety concerns for 2018, and we've pulled together a little chart that shows these top 10 issues.

This list got us thinking about the history of patient safety. How has it improved in a hospital setting over the last decade? What are the areas where there can still be improvement?
One of the top 10 issues that ECRI mentions is “incorporating health IT into patient safety programs.” Specifically, they say, “Facilities should focus on integrating health IT safety into the existing safety program, collaborating with stakeholders, and embedding health IT safety into the organization’s culture.”
While there is obviously much more that hospitals can do to integrate and embed health IT into an organization’s culture, it is also true that hospitals have come a long way over the last 10 years.
Let’s take a look specifically at EHRs. Today, EHRs play a critical role in many health care organization's patient safety programs. Your Clinical Decision Support (CDS) tools are fed from your EHR. Your incident reporting tools, incident auditing tools and retrospective reports all come from data within your EHR. A decade ago, nearly 20% of hospitals were still paper-only facilities (stage zero) and the majority fell at or below stage three EMR use. Until a little thing known as Meaningful Use came along.
Poor Meaningful Use gets a lot of bashing these days. Down with Meaningful Use! Double work! Unnecessary work! Burdensome! Grab the torches … whoops, got carried away there.
But let’s take a look at the progress the nation's hospitals have made since Meaningful Use was initiated.
2008 (Before Meaningful Use)

2017

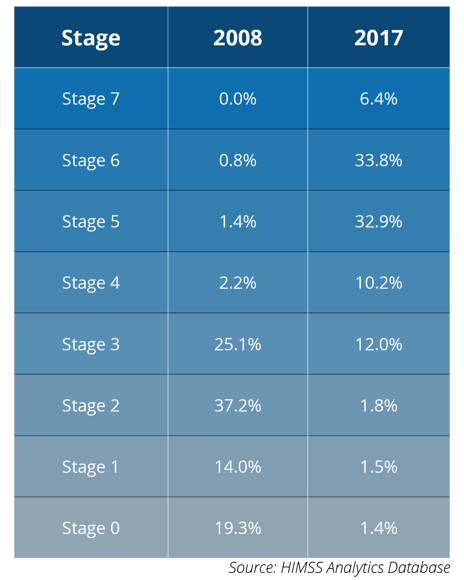
Woah, in only 10 short years all of the numbers have switched around completely. Now, only 1.4% of hospitals remain in the stage zero category, while nearly 34% have climbed to stage six. It is pretty amazing that in 2008 only 2% of hospitals were stage five or above as compared to today, where almost 75% of hospitals have progressed to stage five or above. This adoption is most certainly in direct response to Meaningful Use. Without the incentives to either get additional funds or avoid a penalty, many hospitals may have been much slower to implement.
This increased technology adoption has dramatically reshaped how we think and focus on patient safety. At the lower end of EHR adoption, there isn’t much clinical decision support being used. As hospitals achieve more advanced stages of adoption, they begin to integrate advanced clinical decision support tools into their processes. These can help doctors and nursing staff avoid some patient safety issues by allowing the EHR to remind them of the things they need to consider while treating a patient. As hospitals become more advanced and customize their order sets, this tool can be even more powerful.
It’s not just clinical decision support that is helping hospitals avoid errors and adverse events—an advanced EHR system allows for increased incident reporting and auditing of these events. Many hospitals also use other technology products to improve patient safety. For instance, Medisolv clients use our ENCOR dashboard to look retrospectively at patient safety measures such as the AHRQ Patient Safety Indications (PSI). By dedicating a frequent review of your claims PSI measures, you can begin to identify patterns. Are you trending in a negative direction? Intervene in a timely manner, identify the cause and put actions in place to reverse the negative trend.
Another EHR-related tool that hospitals incorporate into their patient safety programs is the Global Trigger Tool, which is a methodology developed by the Institute for Healthcare Improvement (IHI). This helps hospitals to identify any adverse events a hospital may have experienced. Essentially, each month a hospital randomly audits 20 patient cases to identify adverse events that may have occurred for that patient case. While the technology is meant to help you identify these cases, it also helps you recognize if your organization has a patient safety culture problem. This is a biggie for hospitals. Do your nurses and doctors feel comfortable reporting when they’ve made a mistake? As always, it starts with leadership and creating the correct culture that will make a difference when it comes to your incidents being reported and addressed at the time of the event or discovered a month later, but never reported. Medisolv recently released a tool that helps with automating the Global Trigger Tool methodology.
These last two technology components really only address patient safety in a retrospective way. This is partially what ECRI is commenting on in its report. There is more to do to incorporate health IT into patient safety practices. Many hospitals find it difficult to expend resources and finances to even function at the level we mentioned above. Other hospitals are looking to do even more with their EHR.
Does all of this technology make us inherently better or does it expose us to vulnerabilities?
Ever heard The Notorious B.I.G. rap his famous “Mo money Mo problems” song? Well, implementing an integrated patient safety program with advanced health IT initiatives is kinda like that. As hospital IT departments expand their use of technology to help build out patient safety tools, it empowers teams to succeed, but also creates more opportunities for failure. How are we monitoring for tech errors so they don’t cause additional adverse events? What happens if a hurricane wipes out all of our technology? What procedures do we have in place to avoid patient harm in the case of EHR downtime?
So yeah, more money, more problems. Or as the head of our client services team puts it, “More success, more stress.” He’s still working on his rapping skills.
Download:
2019 IQR Program Requirements eBook
 |





Comments